Disruption of the body’s circadian rhythm promotes tumor growth
A new study from the University of Pennsylvania has found that interference with natural circadian rhythms promotes tumor growth and suppresses the effects of a tumor-fighting drug. The findings highlight the need for “chronotherapy,” which is the delivery of cancer drugs timed to the internal circadian rhythm.
In the background of our brain, a 24-hour clock keeps time for changes in our physical and mental cycles in response to environmental cues such as light and darkness. This natural circadian rhythm regulates many important aspects of our lives.
Disruption of the brain’s circadian clock through sleep disturbances or shift work, for example, is a known risk factor for several types of cancer. While it is known that hormonally-induced circadian disruption promotes tumor growth in animal models, the underlying mechanism has not been clear.
To investigate, the researchers used the hormone dexamethasone to advance daily rhythms in cultured cells. The treatment was found to alter the expression of multiple genes, especially those involved in regulating the cell cycle.
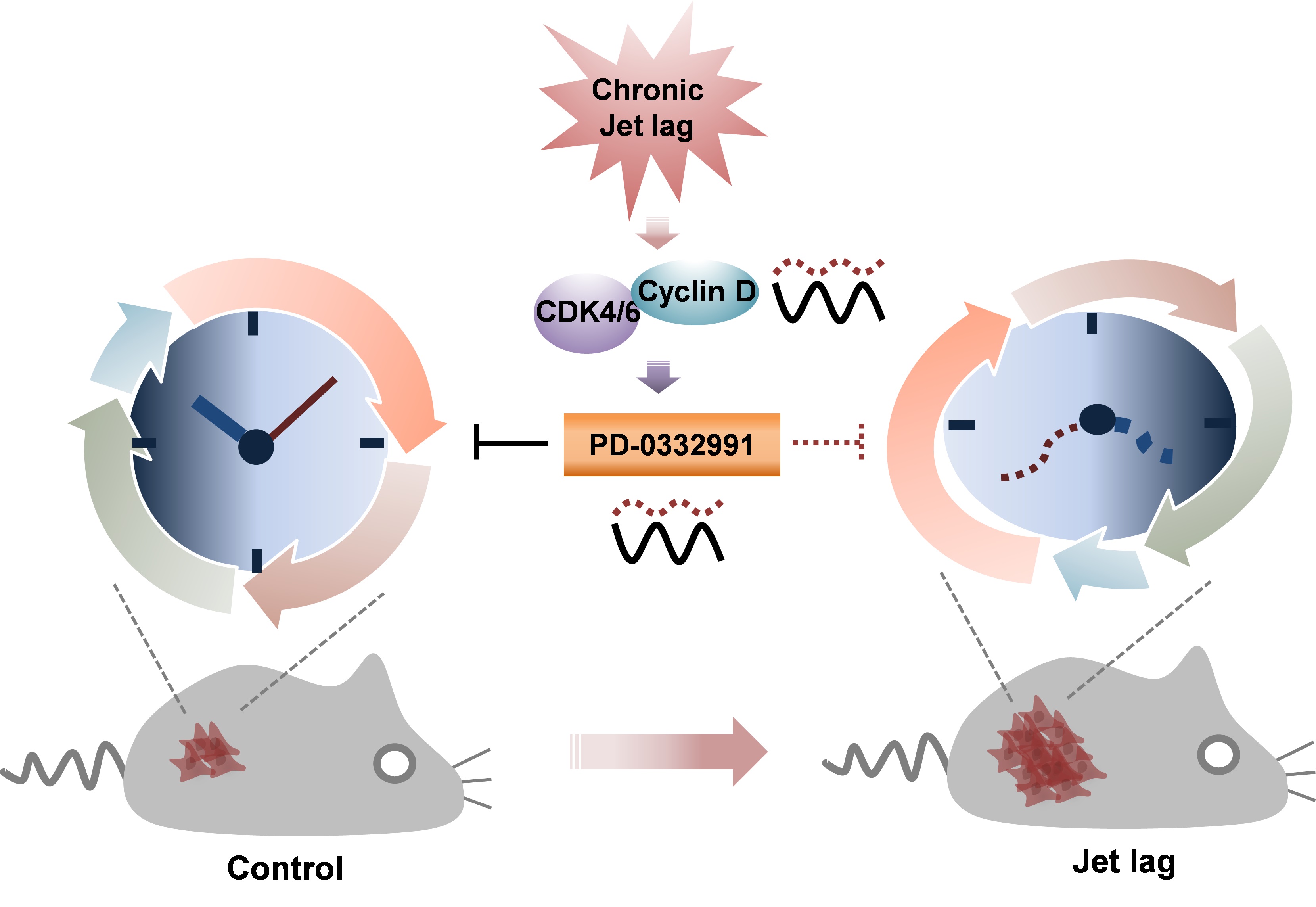
In particular, circadian rhythm disruption increased the expression of a cell-cycle control protein called cyclin D1. This activated cyclin D-dependent kinase 4/6, a step that ultimately leads to cell division.
Tumor growth is closely tied to cell division, so many cancer treatments aim to inhibit the progression of the cell cycle. The researchers found that the tumor-fighting ability of a drug called PD-0332991, which inhibits CDK4/6 activity, varies according to the time of the day.
Essentially, the treatment was found to be more effective in the morning than at night. Furthermore, the efficacy of the drug was reduced in mice when their circadian rhythms were disrupted.
“We suggest that chronic disruption of the normal circadian rhythm tips the balance between tumor-suppressive and tumor-progressive gene expression to favor tumor growth,” said study co-author Amita Sehgal. “Better understanding the molecular effects of jet lag, shift work, and other sources of chronic disruption may lead to strategies to minimize the increased cancer risk associated with these behaviors, and to better treatment strategies, including timing delivery of cancer therapy for maximum benefit.”
The study is published in the journal PLOS Biology.
—
By Chrissy Sexton, Earth.com Staff Writer